Page 50 - Abbott
P. 50
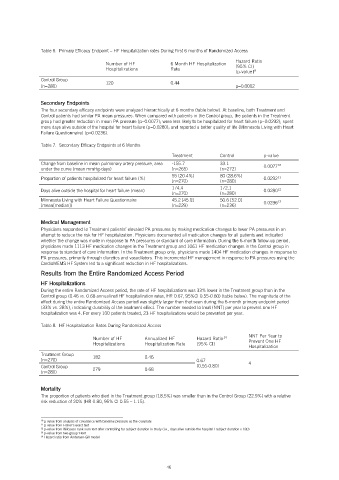
Table 6. Primary Efficacy Endpoint – HF Hospitalization rates During First 6 months of Randomized Access
Hazard Ratio
Number of HF 6 Month HF Hospitalization
Hospitalizations Rate (95% CI)
9
[p-value]
Control Group
(n=280) 120 0.44 p=0.0002
Secondary Endpoints
The four secondary efficacy endpoints were analyzed hierarchically at 6 months (table below). At baseline, both Treatment and
Control patients had similar PA mean pressures. When compared with patients in the Control group, the patients in the Treatment
group had greater reduction in mean PA pressure (p=0.0077); were less likely to be hospitalized for heart failure (p=0.0292); spent
more days alive outside of the hospital for heart failure (p=0.0280); and reported a better quality of life (Minnesota Living with Heart
Failure Questionnaire) (p=0.0236).
Table 7. Secondary Efficacy Endpoints at 6 Months
Treatment Control p-value
Change from baseline in mean pulmonary artery pressure, area -155.7 33.1 10
under the curve (mean mmHg-days) (n=265) (n=272) 0.0077
55 (20.4%) 80 (28.6%)
Proportion of patients hospitalized for heart failure (%) 0.0292
11
(n=270) (n=280)
174.4 172.1
12
Days alive outside the hospital for heart failure (mean) 0.0280
(n=270) (n=280)
Minnesota Living with Heart Failure Questionnaire 45.2 [45.0] 50.6 [52.0] 13
(mean[median]) (n=229) (n=236) 0.0236
Medical Management
Physicians responded to Treatment patients’ elevated PA pressures by making medication changes to lower PA pressures in an
attempt to reduce the risk for HF hospitalization. Physicians documented all medication changes for all patients and indicated
whether the change was made in response to PA pressures or standard of care information. During the 6-month follow-up period,
physicians made 1113 HF medication changes in the Treatment group and 1061 HF medication changes in the Control group in
response to standard of care information. In the Treatment group only, physicians made 1404 HF medication changes in response to
PA pressures, primarily through diuretics and vasodilators. This incremental HF management in response to PA pressures using the
CardioMEMS HF System led to a significant reduction in HF hospitalizations.
Results from the Entire Randomized Access Period
HF Hospitalizations
During the entire Randomized Access period, the rate of HF hospitalizations was 33% lower in the Treatment group than in the
Control group (0.46 vs. 0.68 annualized HF hospitalization rates, HR 0.67, 95%CI 0.55-0.80) (table below). The magnitude of the
effect during the entire Randomized Access period was slightly larger than that seen during the 6-month primary endpoint period
(33% vs. 28%), indicating durability of the treatment effect. The number needed to treat (NNT) per year to prevent one HF
hospitalization was 4. For every 100 patients treated, 23 HF hospitalizations would be prevented per year.
Table 8. HF Hospitalization Rates During Randomized Access
NNT Per Year to
14
Number of HF Annualized HF Hazard Ratio
Hospitalizations Hospitalization Rate (95% CI) Prevent One HF
Hospitalization
Treatment Group
(n=270) 182 0.46 0.67 4
Control Group 279 0.68 (0.55-0.80)
(n=280)
Mortality
The proportion of patients who died in the Treatment group (18.5%) was smaller than in the Control Group (22.9%) with a relative
risk reduction of 20% (HR 0.80, 95% CI 0.55 – 1.15).
10 p-value from analysis of covariance with baseline pressure as the covariate
11 p-value from Fisher's exact test
12 p-value from Wilcoxon rank sum test after controlling for subject duration in study (i.e., days alive outside the hospital / subject duration x 180)
13 p-value from two-group t-test
14 Hazard ratio from Andersen-Gill model
46